WASHINGTON – Scientists have a new lead on a possible treatment to slow Alzheimer’s disease by targeting a protein involved in limiting flexibility in the aging brain, said a study out Thursday.
Alzheimer’s – the most common form of dementia in older adults— affects an estimated five million Americans. There currently is no cure and minimal treatment options exist.
But researchers, led by Stanford University neurobiologist Carla Shatz, hope they can improve outcomes, after discovering that eliminating a certain protein from mice brains stopped the disease’s symptoms from appearing.
“People are just beginning to look at what these proteins do in the brain. While more research is needed, these proteins may be a brand new target for Alzheimer’s drugs,” Shatz said.
The researchers focused on a mouse protein called PirB, and its human homologue LilrB2, which can be found on the surface of nerve cells in the brain.
The protein appears to bind with beta-amyloid – a protein remnant that weakens the connections between neurons.
Experiments showed that when PirB partners with beta-amyloid, it can “trigger a cascade of harmful reactions” that breaks down those connections, the researchers said in a statement.
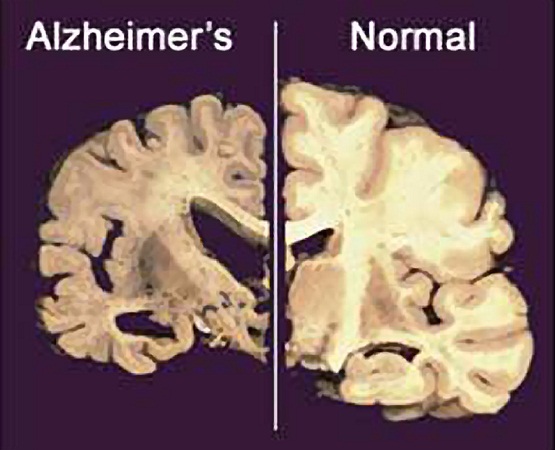
One of the hallmarks of Alzheimer’s disease is large buildups of beta-amyloids called “plaques.”
Scientists say a drug targeting this protein could help slow the progression of Alzheimer’s.
The findings are based on experiments in mice bred to develop Alzheimer’s disease. The symptoms – memory and learning problems— in the mice typically develop within nine months.
Not so in the mice without the PirB gene.
It appears that, without the PirB protein, the mouse synapses were more resistant to the effects of beta-amyloid.
The researchers then examined brain tissue from Alzheimer’s patients, finding the same connection between the human protein LilrB2 and beta-amyloid that they saw in mice.
“These are novel results, and direct interaction between beta-amyloid and PirB-related proteins opens up welcome avenues for investigating new drug targets for Alzheimer’s disease,” said
Roderick Corriveau, program director at the National Institutes of Health’s neurological disorders and stroke center, which helped fund the research.
The findings appeared in this week’s edition of the US journal Science.