Days after the sudden downpour last week, our emergency room filled up again with patients with febrile illnesses. With the imminent rainy season, we just have to brace ourselves for the WILD, which could lead to serious complications, even death.
WILD, an acronym coined by the Department of Health (DOH) a few years ago, stands for four diseases that usually come with the rainy season: waterborne diseases, influenza, leptospirosis and dengue.
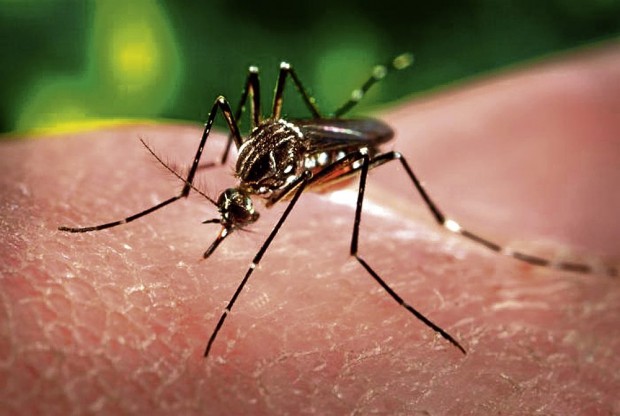
The main causes of WILD diseases are wading in floods, drinking contaminated water, and an increase in the number of aedes aegypti, the dengue virus mosquito vector.
The public must know simple precautionary measures:
1) Boiling drinking water (if bottled water is not available);
2) Washing hands frequently;
3) Using boots when wading in flood water is inevitable, and immediately washing feet thoroughly with soap and water;
4) Avoiding crowded places;
5) Getting rid of potential breeding places for mosquitos;
6) Maintaining a strong immune system by having adequate rest and nutrition.
Influenza
More popularly known as the flu, influenza is a viral infection that can cause temporary injury or inflammation in the lungs, airway and skeletal system.
In most cases, so long as one’s immune system is strong, it is a self-limiting disease. It goes away with just supportive treatment, i.e., rest, hydration and symptomatic treatment of fever, headache, muscle pains.
However, in people with weak immune system, the flu virus can attack the heart, causing it to swell (viral myocarditis). This can lead to heart failure, shown as difficulty in breathing and the feeling of drowning. The brain can also be infected, causing meningo-encephalitis, manifested as severe headache, sensorial changes, disorientation and seizures.
The virus is usually transmitted via direct contact with a person who sneezes or coughs, or coming in contact with surfaces, materials and clothing contaminated with the discharge of an infected person.
Flu is best prevented by avoiding crowded places, covering one’s mouth and nose when sneezing or coughing, and proper hygiene by frequent hand washing.
For those with weak immune systems, having an annual flu vaccine is also recommended.
Leptospirosis
Leptospirosis is a bacterial infection caused by leptospires or spirochetes, usually transmitted when one is exposed to rat urine and feces. This may happen if we wade in contaminated floodwaters. Sometimes, children even swim in them.
The barangay should prohibit such practices, as spirochetes can enter through broken skin and open wounds. Some may get it through the eyes, nose, sinuses and mouth through contaminated water or soil.
One may also get leptospirosis by ingesting contaminated food or water.
One usually experiences the symptoms seven to 14 days after exposure to floodwaters. The symptoms are similar to the common flu, and include fever, muscle pain (especially the calf muscle), and headache. One distinct sign is the appearance of reddish eyes.
Leptospirosis can cause complications in the brain, liver and kidneys. Hence, some people suffer kidney failure and require dialysis.
Liver complications are indicated by yellowish body discoloration (jaundice) and dark urine. Persons developing a flu-like illness one or two weeks after wading in the flood should consult their doctors.
Dengue
Dengue is also caused by virus, and is now a year-round threat in the country. It is a flu-like illness, and a simple blood test can show the platelets, responsible for preventing bleeding in the body, to be temporarily decreased. Again, because it’s also a self-limiting infection in most cases, treatment is supportive, except in those who encounter complications, specifically bleeding.
More than 800,000 schoolchildren have had the antidengue vaccination, and it would be interesting to know if this has reduced the incidence of dengue.
What seems to be more hyped in the media is how many of those vaccinated might experience severe and potentially fatal dengue.
Although the platelet count in the blood has to be monitored, not all cases of dengue should be admitted or confined in a hospital. Dengue without warning signs may be managed on an outpatient basis with close monitoring by the physician up to a week after the fever has subsided.
Complications can happen even after the fever has subsided.
Warning signs include abdominal pain or tenderness, vomiting, mucosal or nasal bleeding, restlessness, marked decrease in platelet count and increase in hematocrit levels. When these are present, it’s better to confine the patient for closer monitoring.
Severe dengue, characterized by severe bleeding, severe plasma leakage leading to shock and respiratory distress, impaired consciousness, signs of liver damage leading to high levels of the liver enzymes (SGPT and SGOT), should be managed in an intensive care unit.
With the dengue vaccination not a recommended preventive measure at this point, focus is on environmental measures, especially getting rid of mosquito bleeding places.
DOH has released the following pointers on how to get rid of breeding places:
Cover water drums and water pails to prevent breeding.
Clean all water containers once a week.
Puncture or cut old tires used as roof support to avoid accumulation of water.
Clean gutters of leaves and debris to prevent rainwater accumulation as breeding places of mosquitoes.
With the rainy season, one can get wet and “WILD.”