The 2019 guideline for the management of dyslipidemias published by the European Society of Cardiology (ESC) in partnership with the European Atherosclerosis Society (EAS), recommended a further reduction in Low-density lipoprotein (LDL-C) or “bad” cholesterol levels, lowering the target up to 50% from baseline for dyslipidemia management.
If the recommended LDL-C level is not reached among patients receiving highest intensity statin therapy, the 2019 guideline recommended adding another non-statin oral therapy, ezetimibe. Ezetimibe is a medication used in the management and treatment of dyslipidemia. It is among a novel class of selective cholesterol-absorption inhibitors.
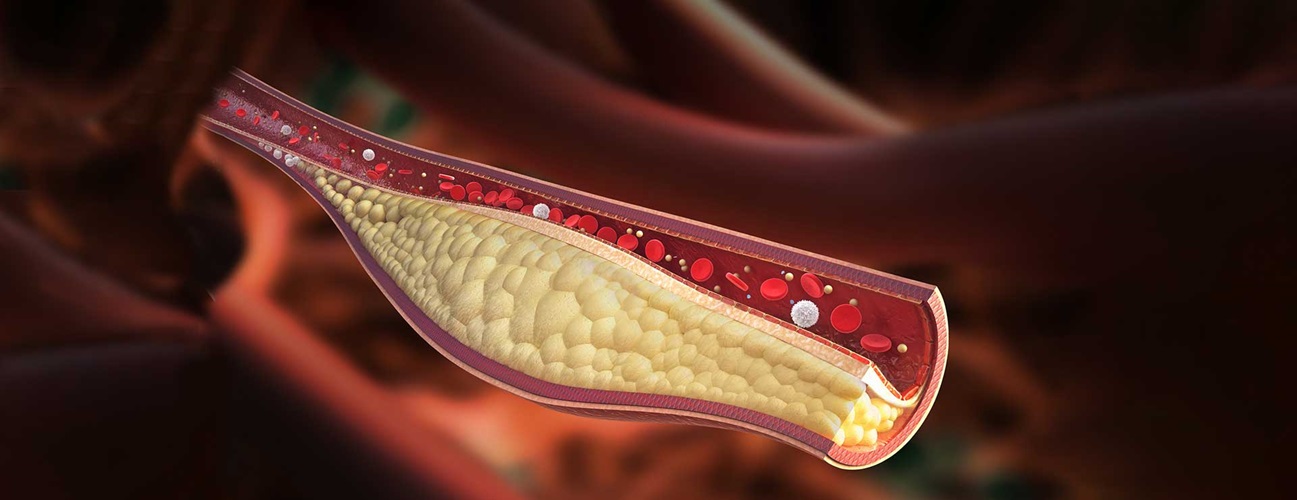
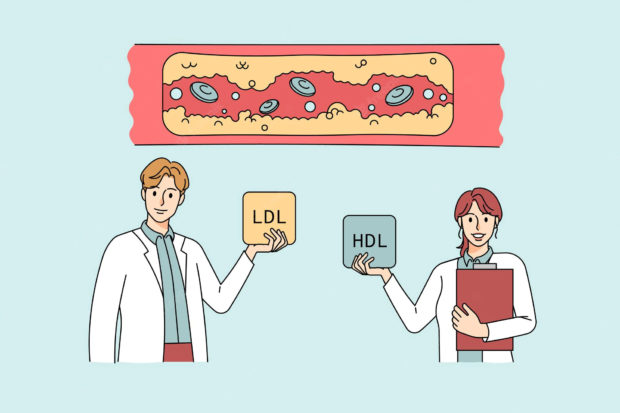
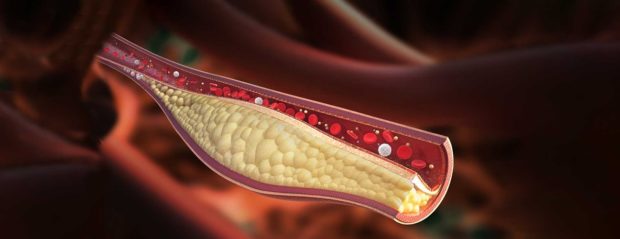
Dyslipidemia is the imbalance of lipids such as cholesterol, LDL-C, triglycerides or a type of fat in your blood that your body uses for energy, and high-density lipoprotein (HDL) or “good” cholesterol. This condition can result from diet, tobacco exposure, or genetics, leading to severe complications of cardiovascular disease (CVD). CVDs can include coronary heart disease, cerebrovascular disease, and other heart and blood vessel disorders.
“The Asia Pacific Region, including the Philippines, has an increase in cases of dyslipidemia, contributing to the development of CVDs. Non-achievement of lipid targets is associated with increased risks of CVD cases and mortality. Those not achieving LDL targets were 32% more likely to die,” noted Dr. Lourdes Ella Santos, Clinical Associate Professor, Dept. of Medicine, UP-PGH.
“LDL-C is the primary treatment target for lipid management. We need to bring our patients to their treatment to goal level; the earlier, the better,” emphasized Dr. Deborah Ignacia Ona, Associate Professor, UP-PGH and St. Luke’s Medical Center.
Moving beyond statin therapy
According to Dr. Ona, current statin therapy for lipid-lowering management practice involves using known statin drugs such as atorvastatin and simvastatin – a reduction of 38% and 23% from baseline, respectively. When LDL-C targets are not met, doubling the statin dose produces an average additional decrease in LDL-C of about 5-6% only.
“We need to be aggressive in lowering the LDL-C levels of our patients. Combination lipid drug therapy is often indicated to avoid known toxicity from higher statin doses,” added Dr. Ona. “Meta-analysis of 19,404 participants from 12 studies who received combination therapy of ezetimibe and statin for a mean duration of 11 months showed a significant reduction in LDL-C.”
“One of the targets of ezetimibe is to block intestinal cholesterol absorption. Three-quarters of cholesterol delivered to the intestine is derived from biliary cholesterol excretion from the liver. Intestinal cholesterol absorption is a clinically relevant mechanism that significantly contributes to hepatic (blood) cholesterol,” Dr. Ona explained.
Dr. Santos illustrated the “rule of 6 limitations”. She said high-intensity statin therapy could reduce up to 50% of average LDL-C. If statin 10mg dose is increased to 20mg or 30mg, this can yield up to 6% LDL-C reduction only. Meanwhile, early introduction of high statin therapy plus ezetimibe can result in a 65% average LDL-C reduction.
“When we talk about treating our patients with dyslipidemia, it’s essential to educate both our patients with that association that if they discontinue statin therapy, they can get a stroke. Physicians also need to understand the importance of treating dyslipidemia and looking at it as one of the risk factors when patients come into the clinic for CVD reduction,” said Dr. Santos.
Recently, a fixed dose combination product comprising of ezetimibe and rosuvastatin was introduced among members of the Philippine Lipid and Atherosclerosis Society (PLAS). “The combination of ezetimibe and rosuvastatin in one pill is a key milestone for the medical community and patients. We are providing an option as the standard of care for patients who failed in statin monotherapy to achieve their LDL-C target with ease, and help in aggressive LDL-C lowering strategies for lowering the risk of CVD events,” shared Mr. Emman Tiglao, Organon Commercial Director in the Philippines.
By identifying an individual’s risk of CVDs and ensuring access to cholesterol medications, Organon maintains its commitment to delivering impactful medicines and solutions for a healthier every day. The healthcare company is working to effect positive change globally by listening to patients about their healthcare needs.
ADVT