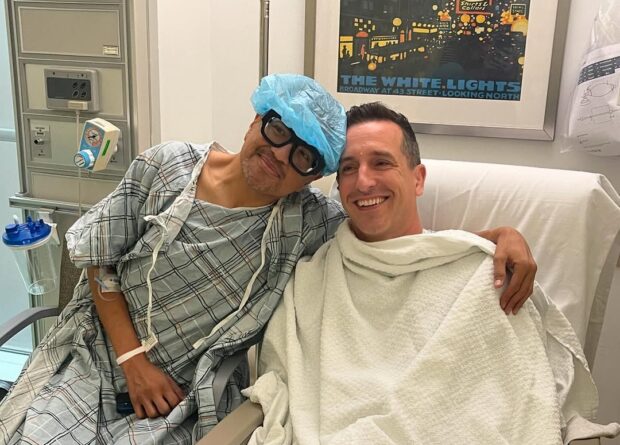
The photograph of breast cancer patient Irene Lee sitting quietly in a chair along a corridor in Makati Medical Center (MMC) appears strangely eerie, as Lee herself admits, because the normally bustling hospital appears deserted.
“When I started chemotherapy infusion in June, the hospital was quiet,” says the accountant, management consultant, and wife and mother. “So weird that I took pictures of the empty halls. Nowadays, there are more people going back for treatment. It feels safer now, because I never once saw any of the staff being lax in donning their personal protective equipment (PPE). The patients are also put in individual sanitized rooms while undergoing infusion.”
Lee—who, as of this email interview, had just completed her fifth session of chemotherapy, and may have just one more to go—has been on a long breast cancer journey. First diagnosed in 2005, she completed “the whole nine yards” of chemotherapy and radiation. In 2009, another breast mass led to a mastectomy and reconstructive surgery, but the implant had to be removed when her body rejected it.
Just this January, a checkup revealed yet another mass. “My breast cancer cells had migrated to my liver,” Lee recalls. “I was momentarily sad, but there was no sobbing over the diagnosis, unlike in 2005. I am now stage 4 at 54 years old… Now, I am incredibly determined to complete all treatments, unless I want to face the risk of this disease migrating again.”
If Lee sounds brave, that’s because she may be even braver than we think: She was among very few breast cancer patients who opted to continue treatment even throughout the COVID-19 pandemic.
High-risk cancers
In a webinar held by the breast cancer support group, ICanServe Foundation Inc., on Sept. 5, titled “Staying Safe: Cancer in the time of COVID-19,” Dr. Ellie May Villegas, past president of Philippine Society of Medical Oncologists (PSMO) and section head for medical oncology at Cebu Doctors University Hospital, confirmed some sobering statistics.
“According to PSMO surveys, more than 50 percent of patients have had recurrence and progression of the disease, or have even died, not because of COVID-19, but because of delay in treatment. Worldwide, as of June 2020, some 10,000 cancer patients have died because they skipped treatment.”
Breast cancer patients are considered among those with high-risk cancers when diagnosed in more advanced stages, or if they fall within certain parameters such as having her2-positive breast cancer (that is, they have tested positive for a protein that makes their cancer aggressive) or triple negative breast cancer (when the cancer cells have no estrogen or progesterone receptors and tend to spread faster, leaving the patient with fewer treatment options).
“People go out for their ‘essentials,’” Dr. Villegas noted, “but they forget that among these essentials is to have chronic diseases checked regularly.”
The noncompliance at the beginning of the lockdown was “not unexpected,” says Dr. Maria Luisa “Malu” Tiambeng, director of the Cancer Center of Cardinal Santos Medical Center, who has been treating breast cancer patients for 20 years. “The fear was crippling everyone, and at a heightened degree for cancer patients, given their vulnerable state.”

Oncologists had their own fears during that time, Dr. Tiambeng reports. “First, we were concerned that patients with potentially curable diseases were not being diagnosed early enough to achieve that goal. At the start of the pandemic, outpatient clinics were closed, and our surgeons were not allowed to perform biopsies and mastectomies during the enhanced community quarantine (ECQ). So even though our cancer center remained open, no new patients were being diagnosed.”
Dropout
Second, says Dr. Tiambeng, there was the possibility that patients who had already started treatment, but chose to delay it for fear of contracting COVID or because of logistical issues, would lose the benefits of the treatment they had begun. This was a more common problem among patients in government hospitals, due to lack of public transportation.
“Third, we were concerned that we were losing our stage 4 cancer patients, who were otherwise responding to treatment, due to dropout,” Dr. Tiambeng continues. “To quantify these concerns, in a recent survey conducted by PSMO among 92 medical oncologists, 85 percent of respondents said their patient census decreased since the pandemic started, and 93 percent said their patients delayed their treatment, from one month to even beyond four months. This happened despite 97 percent of medical oncologists saying their cancer centers remained open to deliver cancer care services during the lockdown.”
The sad part is, the fear may have been largely unfounded, it seems. “Of these doctors who continued to see patients, 83 percent said none of their patients contracted COVID while having their treatment,” says Dr. Tiambeng. In the webinar, Dr. Villegas cited July 2020 studies from the University of Birmingham that indeed, cancer patients were not particularly immunocompromised, unless they had comorbidities, such as diseases like hypertension or diabetes, or unless they were among the elderly.
“I was trying to mitigate any further metastasis,” Irene Lee says simply when asked why she opted to soldier on. “As it is, the liver metastasis of my breast cancer is already difficult to cure. I am confident, though, that with the guidance of my doctor daughter, Chelsea, we are exercising enough stringent methods to avoid getting the virus.”
‘My choice’
For her oncologist, Dr. Mabel Tamayo, it was not even a question of pursuing treatment or not, Lee says, “but how to create the right cocktail of treatment for me. We have this agreement that I will come to MMC when needed, and she will be present for me virtually or physically during chemotherapy, too.”
After chemotherapy, Lee recounts, she confines herself to her room to avoid being exposed to any possible COVID carriers. For two weeks after each session, she is served meals in her room. “I bought a smartwatch that acts as a monitor for heart rate, oxygen saturation and sleep patterns, and as a pedometer. Pre-COVID, I used to walk in the village at night and would be happy if I clocked 45 minutes or did 4,000 steps. Nowadays, I clock 6,000 steps walking around my room.”
“We advised our patients who were on chemotherapy or who needed to start chemotherapy to go on with their treatment as scheduled, as this will have an impact on their survival,” Dr. Tiambeng says. “For those who just needed to be followed up on because they were on oral chemo or had completed chemo, we asked them to use telemedicine, which we have made available both in private and public hospitals.

“For procedures which could be delayed, such as an annual mammography or biannual bone infusions, we gave the patients an option to wait until the situation became more controlled. Patients who were able to reach us generally followed our recommendations, but the problem was with patients who just chose not to follow up at all.”
‘Cancer does not sleep’
As a final word, Dr. Tiambeng asks breast cancer patients, “Please reach out to your medical oncologists in whatever way possible, be it via face-to-face consults or telemedicine. We are here for you. We have instituted measures in our cancer centers to ensure your safety. Cancer does not sleep, and will not go away despite the pandemic. Please do not surrender your chance for a cure or a better quality of life because of COVID.”
“I shared with my famly my intention to do everything humanly possible to overcome this illness,” Lee says. “I believe that God is running the show and knows how each of our stories will play out. In the meantime, while I am pursuing my treatment, I will enjoy every moment I wake up in the morning to start another day.”
This fighter’s advice to women who stopped treatment for fear of COVID: “It’s just an additional nuisance that adds to your logistical demand for care. Do not expend energy debating about PPEs; just follow what is needed. Be thankful to immediate family members if they are supportive, because caring for a cancer patient is also not easy.
“Patients should not let COVID play a major role in their lives, just like patients should not let cancer play the starring role. These are just parts of the life of a patient—and the whole is always greater than the sum of its parts.” INQ