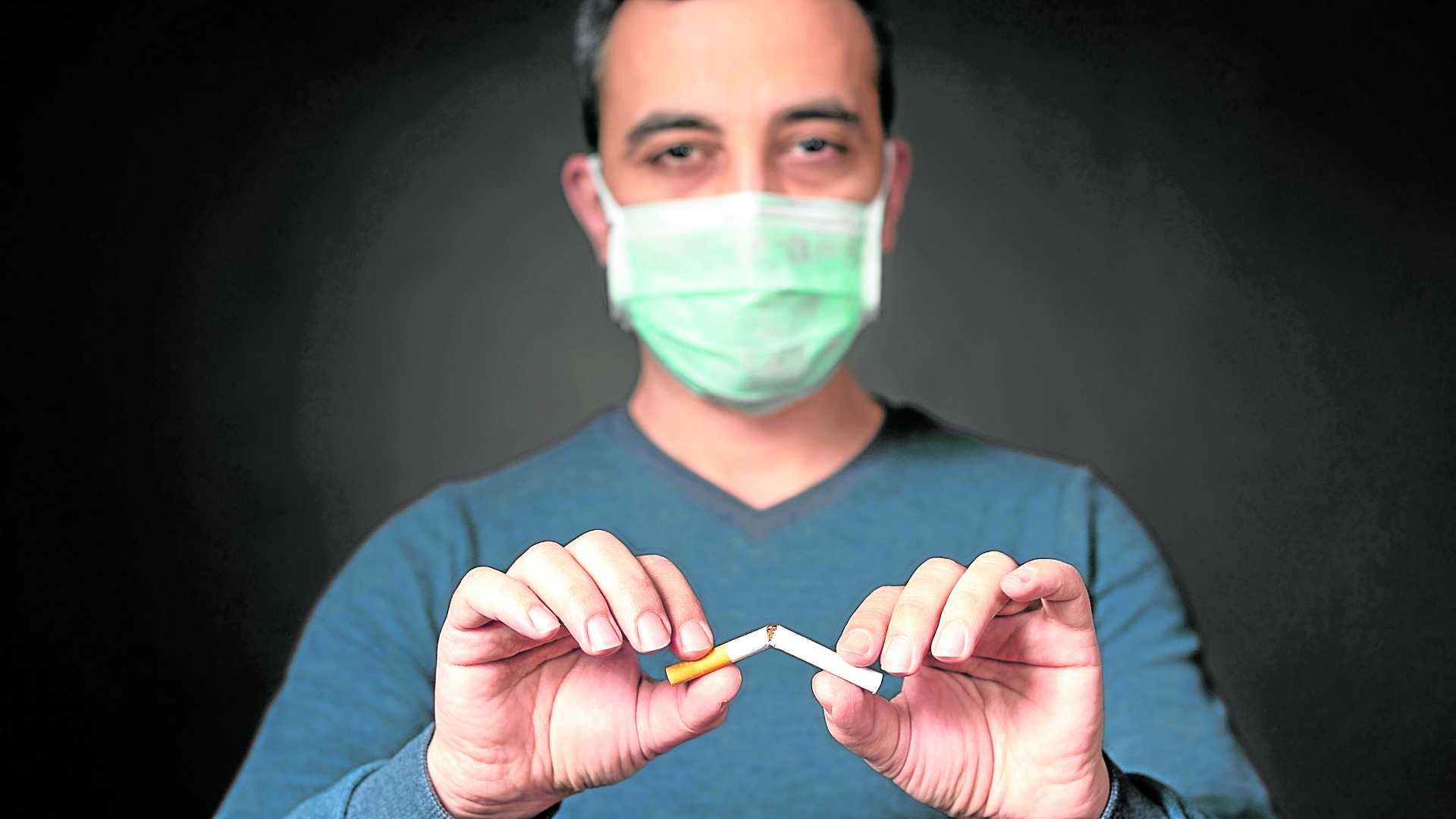
This pandemic highlights the urgent need for active smokers to quit smoking or shift to a less harmful alternative to prevent smoking-plus-COVID-related complications. —integrisok.com
Nothing can be more frustrating for a physician than to be bluntly told by a recalcitrant smoker that “his spirit is willing but his flesh is weak.” In short, he simply could not lick the vice.
The sense of helplessness grips not only the smoker, but the physician, as well, who may have exhausted all means and interventions—from gums to patches to counseling—to make the smoker quit.
We define recalcitrant smokers as those who have an obstinately uncooperative attitude toward smoking cessation. Initially, they may show genuine efforts of cooperating with the smoking cessation programs we practice in our clinics, but this enthusiasm is short-lived; the urge to puff reigns (“Just one puff!”), and he slides back completely. There is simply a lack of perseverance and will to persevere and persist until the end goal of complete smoking cessation is achieved.
We feel bad about our 30-percent success rate at smoking cessation, realizing that we fail in seven out of 10 of our recalcitrant smokers. But when we read that the success rate in smoking cessation interventions in even well-supported programs is less than 15 percent, somehow we feel comforted that we’re not an utter failure in reducing the health risk of our smoker patients.
However, the big question remains: What can we do for the big majority of smokers who simply could not quit, despite best efforts from him (the recalcitrant smoker) and his physician? Do we just leave them to fend for themselves until a serious complication, including severe COVID-19, hits them?
Nonnegotiable
After decades of clinical practice dealing with problematic smokers, including those who remain smokers despite their bad hearts and lungs and other smoking-related complications, we wrote a perspective commentary with review of relevant literature, chronicling our change in perspective in dealing with these recalcitrant smokers.
Stopping smoking used to be a nonnegotiable requirement for our heart patients to remain in our clinic’s roster of patients beyond the six months they were given to lick the vice for good. After six months, if they continue to smoke, they’re “expelled” from the clinic and referred to other clinics for followup.
After several weeks of peer review, the Cardiology and Cardiovascular Medicine Journal published our paper on Nov. 15 on the interventions and alternatives we could offer recalcitrant smokers, to mitigate their cardiovascular risk, especially in the context of the current pandemic.
In the paper, we cited studies about how the current pandemic has highlighted the great risk active smokers are unwittingly exposing themselves to. There is an increased propensity for active smokers to develop severe COVID-19 should they get infected with the virus.
Reddy et al. analyzed 47 studies enrolling 32,849 symptomatic and hospitalized COVID-19 patients. More than one-fourth (25.3 percent) in this large pool of patients had a smoking history, associated with a higher risk to develop severe COVID-19 and worse in-hospital outcomes. As expected, in the group who were active or current smokers, the risk was highest.
It is now well-known that COVID-19 can also trigger blood clots and inflammation (swelling) of the arterial lining, leading to heart attacks, strokes. There’s some evidence suggesting that these complications are much worse in smokers.
We can’t help it sometimes—we tell our recalcitrant smokers that if they’re not afraid of heart attacks, strokes and cancers, they should be afraid of getting severe COVID-19, getting intubated and hooked to mechanical ventilators (breathing machines), incurring millions in hospital expenses and leaving their families with a huge amount of debt. It’s a puzzle why many still seem to brush off these risks and continue to smoke.
In these recalcitrant smokers, it’s either you give up on them completely or offer them some alternatives which may at least reduce their health risks. This is where alternative tobacco products (ATPs), including heated tobacco products (HTPs), may play a role.
Less amounts
Even the World Health Organization (WHO) Study Group on Tobacco Product Regulation has reported that compared to cigarette smoke, aerosols from heated tobacco contain less amounts of harmful chemicals such as tobacco-specific nitrosamines and carbonyl compounds, which are well- known for their harmful effects.
By no means are these HTPs safe but compared to cigarette smoke, they’re likely to be less harmful, and recalcitrant smokers are better off with them than continuing to burn and smoke cigarettes.
We wanted to validate this information ourselves and not take other researchers’ word for it, so our group consisting of Dr. Ma. Joan Dymphna Reaño, Dr. Marie Barrientos-Regala and Reginald Arimado and myself—all members of the Cardio-Metabolic Research Unit (Cameru)—conducted two independent systematic reviews and meta-analyses. We looked at the effects of both conventional cigarettes and HTPs on cardiovascular risk factors biomarkers of exposure (toxic inhalants).
In the first meta-analysis we conducted, with Barrientos-Regala as our primary author, HTPs showed significantly less negative or harmful effects compared to conventional cigarettes. There were indications of better blood flow, higher level of good cholesterol (high-density lipoprotein) and slower heart rate in those on HTP.
A fast heart rate, which smokers tend to develop, can be just as harmful as a higher blood pressure since it increases the oxygen demand of the heart and can lead to a heart attack in those with clogged arteries.
In the second meta-analysis with Reaño as our main author, we compared the known toxic inhalants or biomarkers of exposure (BOE) resulting from conventional cigarettes and HTPs.
Burnt cigarettes are known to produce more than 7,000 toxic chemical substances associated with smoking-related diseases such as lung cancer, cardiovascular diseases, and chronic lung diseases like emphysema.
In this study, it was shown that there were significantly lower levels of BOE in those on HTPs.
In his Opinion column in this paper, Peter Wallace also highlighted the need to look at the smoking problem with a broader perspective (“Let’s reduce the deaths,” 11/25/21). He proposes a pragmatic middle ground for smokers by switching to alternative tobacco products and, at the same time, making sure the youth are kept away from these products.
It’s good to note that the number of smokers worldwide has slowly decreased in the last few years—from 1.32 billion in 2018 to around 1.3 billion as of latest report. This represents a mere 2.5-percent reduction of the total number of smokers that have quit in the past two years or 1,0250,000 less smokers per year.
This may be a positive direction, but the number of smokers is not going down fast enough. We know there’s no quick fix to it, but a pragmatic and aggressive approach to the problem that shows some promise in mitigating the outcomes should be tried. The use of ATPs and HTPs may be one such approach.
In our clinics, we emphasize that permanent smoking cessation is still our main goal but as a mitigating measure, we allow our recalcitrant smoker patients to shift to HTPs as a relatively less harmful middle ground.
However, there’s a conscious effort to constantly remind them to give up smoking eventually.
Still evolving
The science on HTPs is still evolving. The data is still limited and not sufficient to make definitive conclusions about the benefit or harm of HTPs and the other ATPs. As we pointed out in our published commentary, even treatment guidelines recognize the equipoise, and encourage being on the side of caution, since there is still “insufficient data” to either recommend or advise against HTPs.
According to the WHO, “there is no available evidence to conclude whether HTP use is associated with any long-term clinical outcome,positive or negative, from exposure to the mainstream or secondhand emission.”
From our perspective though, it’s fair to assume that HTPs are at least not as harmful as conventional cigarette smoking.
Our group in the Cameru has made a commitment to try to contribute to the science and find out if HTPs and other ATPs are really a boon or bane to our recalcitrant smokers. We hope other researchers in the country and in other Asian countries can also conduct similar independent studies. After all, smoking is considered the No. 1 risk factor accounting for the most number of deaths in the region and many parts of the world.
Though we support the use of HTPs in recalcitrant smokers, we share the concern about its potential for abuse, especially by our youth.
This is where effective legislation can provide the necessary control measures. Not only the youth should be protected but even older nonsmoking adults, especially the women, who could be lured into the vice.
Senate Bill No. 2239 and House Bill No. 9007, which aim to regulate nicotine products, should provide the needed controls, but they should not be more stringent than what is currently imposed on conventional cigarette products, or else the enacted laws could be self-defeating and may make inaccessible the pragmatic middle ground. INQ